Herpes Virus Infection in Pregnancy
If someone says the word “Herpes”, everyone cringes. Surprisingly, about 2/3 of you reading this now, may have had HSV 1 (the type that causes cold sores), and about 20% of you may have had the genital type of Herpes (HSV2). Most people who get exposed to herpes are asymptomatic and may not even know they had it. The way we can tell if you have been exposed to this virus before is to measure your immunoglobulins (IGG) against the herpes virus.
Most episodes of HSV during pregnancy are recurrent, and are a very low risk to affect the baby. Transmission occurs through mucous membranes or open or abraded skin. The virus lives in the neurons where it entered near the spine. Recurrent clinical outbreaks occur infrequently, and may involve trauma, UV radiation, change of temperature, pregnancy,stress, immunosuppression or hormonal changes.
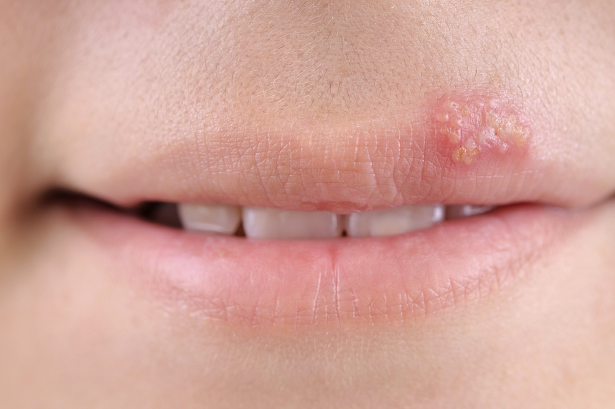
Infection presents with papules, pustules, vesicles and ulcers that last 2-6 weeks
The fetus becomes infected by a virus shed from the cervix or lower genital tract. It either invades the uterus during membrane rupture or is transmitted by contact with the fetus during delivery. Neonatal herpes is caused by both herpes simplex types 1 and 2, although herpes simplex type 2 infection predominates. Most infected infants are born to mothers who have no reported infection.

How it affects You/Pregnancy?
The risk of neonatal infection correlates with the presence of HSV in the genital tract, the stage of maternal infection and invasive obstetrical procedures. If the pregnant woman acquires a new infection near the time of delivery the infant has a 30- to 50- fold increased risk of infection due to higher viral load and the lack of protective antibodies. While women with recurrent HSV have less than a 1-percent risk of neonatal infection.
How it affects the mother?
Only 1/3 of newly acquired Herpes infections are symptomatic. The incubation period of 2-10 days followed by eruption that is papular with itching and tingling, which then becomes painful and vesicular. Transient flu-like symptoms are common. Although very rare, life threatening herpes infection may develop in the mother (disseminated disease) with encephalitis, hepatitis and pneumonia may develop. All signs of infection disappear in 2-4 weeks. Many women do not present with the typical lesions, some may have pruritic or abraded areas others may have knife-slit lesions that may sting, or be itchy.
How it affects the baby?
Neonatal transmission occurs during pregnancy in about 5% of cases, during labor and delivery around 85% and after delivery around 10%.
The most concerning HSV infection during pregnancy occurs in those with a primary/first episode infection in early pregnancy. These are associated with an increased risk of preterm labor, IUGR (intrauterine growth retardation), spontaneous abortion or stillbirth. Premature infants account for 2/3 of the cases of neonatal HSV.
Late-pregnancy infection has been associated with preterm labor and delivery. 80% of mothers of infected infants have no reported infection. This often occurs because the mother is unaware that she was infected, or exposed to a partner with HSV. Epidemiologic studies suggest that most sexual transmission of genital herpes occurs when persons shed virus but lack lesions. Both men and women can shed the virus, without visible lesions on their genitals.
Primary/first episode infection during pregnancy is associated with microcephaly and neonatal chorioretinitis; rarely skin lesions. The risk of fetal transmission with HSV primary infection is about 60%. 20% of those with neonatal HSV have long-term neurologic sequelae.
Treatment and Prevention
Specific antiviral medications have been used successfully to attenuate the infection and reduce viral shedding. In those women with a history of prior HSV (recurrent HSV), and recurrent outbreaks, suppressive therapy with daily antiviral treatment has been used successfully to reduce outbreaks, decrease viral shedding, and decrease neonatal HSV.
Antiviral treatment with medication such as Acyclovir appears to be safe in pregnant women.
If women at term with a history of HSV, present with prodromal symptoms of HSV infection such as vulvar burning or itching, and careful examination of the vulva, vagina and cervix should be done to evaluate for the presence of lesions. Cesarean section is indicated for those with only active genital lesions or prodromal symptoms. However even after cesarean section, some infants are born with HSV. Postnatal treatment with antiviral medications are
given for neonatal herpes infection.
This post was presented to you by VSacharMD.com The World’s first and only cosmetic company devoted to safe, non-toxic cosmetics in pregnancy. Toxin exposure in utero is associated with adult diseases as the child grows such as cancer, diabetes, and more.Prevent exposure to toxins by using safe, non-toxic cosmetics.
Copyright 2014 V Sachar MD. All Rights Reserved.